SIS Insights Blog
Designing a Roadmap to Improve Verifications for Benefit Programs in California
December 2018 | Blog
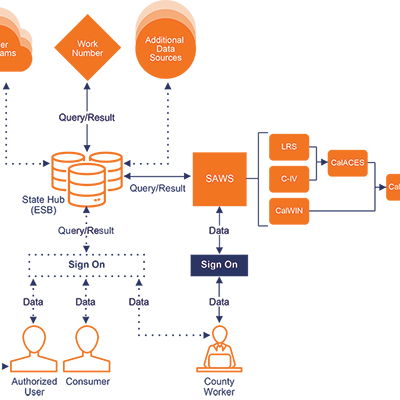
What are the challenges faced by clients and staff when people apply for benefits, and how can they best be remedied? To answer those questions, SIS has completed an extensive policy and technical analysis of the existing verification process used by CDSS when individuals and families apply for CalFresh and CalWORKs.
Read More Social Interest Solutions is a leader in leveraging cutting-edge technology to improve access to critical programs and services for low-income individuals and families.
Social Interest Solutions advances federal, state, and local policies to streamline and modernize eligibility and enrollment processes and improve consumer access to health and social services programs.